A 1st ‘Platform’ Trial, Data Hub for Research, and Other Advances in ALS: Talk With MDA
Written by |
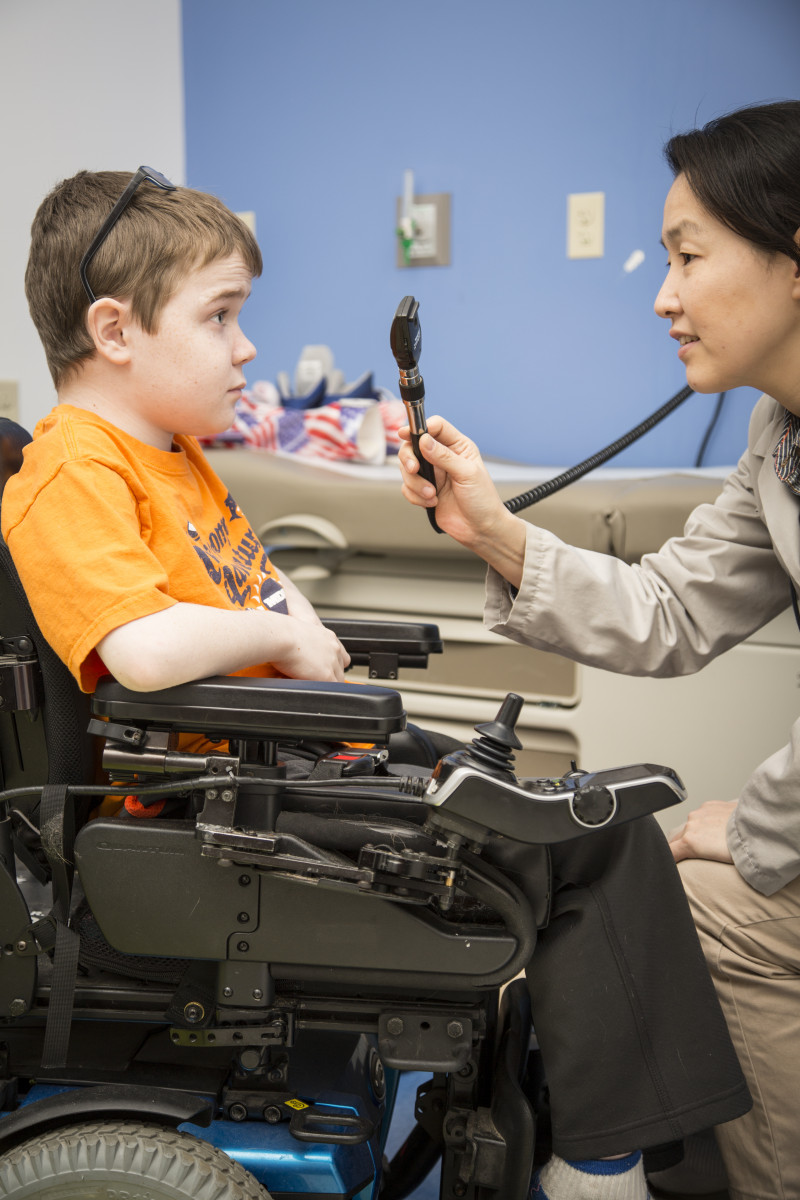
A child being examined at an MDA care center. (Photo courtesy of the MDA)
Much work is ongoing in amyotrophic lateral sclerosis (ALS), as researchers look for better ways of treating people with a disease that progressively cripples and kills motor neurons — and possibly finding a first therapy addressing the root cause of ALS rather than its symptoms.
“ALS is always a really active area, there’s a lot going on,” said Sharon Hesterlee, PhD, an executive vice president and chief research officer for the Muscular Dystrophy Association (MDA) in an interview with ALS News Today. “We have 42 active ALS grants now, and a combined over $10 million in funding.
“Because it’s not in our name, people don’t realize that we have a really significant commitment to ALS. It’s close to half of our [research support] budget,” added Hesterlee, who has a more than 20-year career in the pharmaceutical and biotech industries as well as nonprofits (including with the MDA, where she worked in drug translation and venture philanthropy from 1998 to 2009).
Since its founding in 1950, the MDA has invested more than $1 billion in research into the 40 distinct, and often rare, neuromuscular diseases it covers. The nonprofit awarded $16.8 million in direct research grants in 2019, part of a total $66 million multi-year funding commitment, and anticipates giving out about $18 million in grants in 2020.
Existing treatments largely target symptoms that range from widespread and progressive muscle weakness (including for respiration and swallowing) to spasticity (stiffness), fatigue, anxiety, and depression.
Work in new symptomatic treatments is underway, including Ultomiris (ravulizumab) by Alexion Pharmaceuticals, which is approved in the U.S. for two blood disorders. Ultomiris prevents overactivation of the complement system, a part of the immune system thought to be implicated in neurodegeneration in ALS, and may be able to slow disease progression. The drug will be tested against a placebo in a Phase 3 trial (NCT04248465), called CHAMPION-ALS, that’s expected to begin enrolling more than 350 patients in March.
But early research is also of interest to the MDA. Among these preclinical efforts is work into the metabolism of lipids (fat molecules), whose imbalance can affect motor neurons. Such an imbalance could result from a loss of C9orf72, a protein whose corresponding gene is among those most often mutated in familial ALS.
Or it could come from rising levels of lipids and their altered metabolism (chemical reactions in the processing of lipids for cellular energy and health), possibly as a defense against oxidative damage. ALS patients are known to have higher amounts of specific lipids — ceramides, glucosylceramides and phosphatidylcholine — in their cerebrospinal fluid, the liquid surrounding the brain and spinal cord, a study reported.
More immediately promising, Hesterlee said, are signs of cooperation coming to the fore across pharmaceuticals, research institutions, and nonprofit patient groups — of which the HEALEY ALS Platform Trial and patient databases such as MDA’s MOVR Data Hub are timely examples.
“It really does make sense that you want to bring as many resources together as possible in rare disease spaces. You can’t duplicate resources,” Hesterlee said, speaking of HEALEY, a first multi-drug, or platform, study for any neuromuscular disease.
There’s also “less rivalry” with information collected from or given by patients, and that’s a huge leap, she said. “People are starting to share the datasets they used to horde. I think all of this … bodes well for the future.”
HEALEY, a first in trials for ALS
Studies in patients typically test one potential treatment at a time, often against placebo as trials shift into pivotal stages and prepare to request approval from regulatory agencies.
But companies and groups working in oncology began to use a variety of “master protocol trials” as treatments became more targeted in the 2010s, testing several drugs in parallel with allowances for new treatments and patient groups to be added — or dropped — as their platform trial progressed.
The savings could be enormous, in the time and money spent designing and vetting individual studies for each treatment that had promising lab and animal work.
“You’re not duplicating all of that infrastructure every time you have a different drug. You’re using the same protocol,” Hesterlee said.
HEALEY was conceived in 2018 by neurologist Merit Cudkowicz, MD, and neuroscientist Sabrina Paganoni, MD, PhD, both with the Sean M. Healey & AMG Center for ALS at Mass General, in partnership with online fundraiser Tackle ALS.
It was launched one year later, and a request for proposals brought in nearly 30 applications from 10 countries, Mass General reports in a presentation.
Five were chosen for inclusion at the trial’s opening, expected in May or June, Hesterlee said.
Three were recently given FDA approval for use in the platform trial: zilucoplan, by Ra Pharma, a small molecule also working against complement system overactivation; CNM-Au8, by Clene Nanomedicine, a liquid suspension of gold nanocrystals aiming to improve nerve cell survival and function; and verdiperstat, by Biohaven Pharmaceuticals, an oral small molecule that works to lower inflammation and oxidative stress in the brain and spinal cord.
A primary goal for each treatment will be changes in disease severity after six months, as assessed by the ALS Functional Rating Scale-Revised, which is a measure of daily life activities, from speaking and swallowing to cutting food, walking, or climbing stairs.
About 160 patients — broadly representing ALS — are reportedly planned for each treatment group, and some will be randomly assigned to a sham group. But far more people than is typical for pivotal trials will be treated, with three patients going to an active (investigative) trial arm for every one assigned to a placebo arm.
Enrollment is likely to open soon, with 54 centers across the U.S. expected to take part.
“Therapeutics [in ALS and other neuromuscular diseases] are often complicated and expensive,” Hesterlee said. “It’ll be interesting to watch as this platform trial gets underway.”
MOVR and MDA clinical care centers
The MDA runs a network of neuromuscular specialist care centers at more than 150 clinics across the U.S. (with at least one in each state), which average about 55,000 patient visits each year, Hesterlee noted.
“We have long-standing relationships with the centers and their directors and staff,” she said. “It was sort of a no-brainer to set up a database and start collecting data at the point of care in the diseases that we cover.”
This effort actually began in 2016, but a decision was made to transition to a more sophisticated platform about a year ago.
The result is the MOVR Data Hub (for neuroMuscular ObserVational Research), jointly operated by the MDA and the contract research organization IQVIA.
Data capturing disease, diagnostic, and encounter information over time, collected by both clinicians and patients, is being fed into MOVR, adding to the “legacy data” from the previous three or so years, Hesterlee said.
To date, seven neuromuscular diseases — ALS, Duchenne muscular dystrophy, facioscapulohumeral muscular dystrophy, Becker muscular dystrophy, limb-girdle muscular dystrophy, spinal muscular atrophy, and Pompe disease — are included, covering about 4,000 people.
Expansion into the 33 other diseases under the MDA umbrella is planned, with about 40 care centers already approved to take part and another 40 working through the process.
Patients or treating clinicians can request to participate in MOVR, but signed consent is required and patient data carefully protected. It’s “highly curated, very high quality data with good quality assurance,” Hesterlee said, and compliant with federal regulations necessary for regulatory filings.
“We would like to see every patient seen at an MDA site with a platform have the opportunity to participate,” said Kristin Stephenson, chief of advocacy and care services and an executive vice president with the MDA.
Most important is how the information contained in MOVR might help both treating doctors and active researchers. Potential uses range from comparing patient responses and outcomes across clinical centers to helping investigators with questions about endpoints or progression in a rare disease, Hesterlee said.
“Industry is certainly interested in using the data for feasibility studies for clinical trials — like establishing eligibility criteria — and a potential interesting use is as a comparator for a placebo arm” in a study in patients.
“In rapidly progressing, serious diseases, it’s really hard to have a placebo group,” she added.
Stephenson said that each of these diseases “are rare diseases by definition, and some very, very rare in terms of the total population living with the disease. So, the reality is that you can have a smaller cohort that can still yield very meaningful data.”




Leave a comment
Fill in the required fields to post. Your email address will not be published.