New Strategy May Prevent Toxic Protein Aggregates Linked to Neurodegenerative Disorders, Study Suggests
Written by |
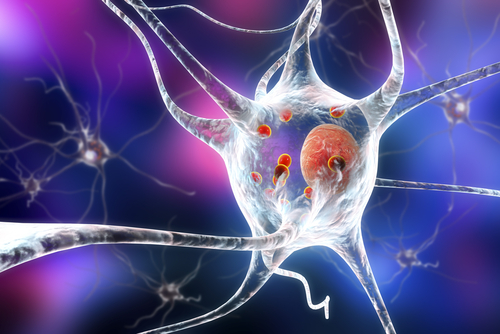
A modified experimental version of the TDP-43 protein has revealed the underlying mechanisms that support its accumulation and the formation of toxic aggregates implicated in amyotrophic lateral sclerosis (ALS) and frontotemporal dementia (FTD), a study reports.
A detailed understanding of TDP-43-mediated neurotoxicity may help researchers find new targeted strategies to prevent and manage these progressive neurodegenerative disorders.
The newly identified TDP-43-related cellular mechanisms were reported by researchers from the University of Pittsburgh and their collaborators in a study titled “RNA Binding Antagonizes Neurotoxic Phase Transitions of TDP-43,” published in the journal Neuron.
Approximately 97% of ALS cases and 45% of FTD cases exhibit a common neurological feature known as TDP-43 proteinopathy, which is characterized by the accumulation of TDP-43 proteins in nerve cells.
This protein regulates gene levels and also ensures that the correct genes’ sequence is properly read. Genetic variants of the TDP-43 protein-coding gene, TARDBP, have been linked to cases of familial ALS, strongly suggesting that this protein contributes to the development of ALS.
Given the importance of TDP-43 as a critical convergent feature of several neurological disorders, improved “mechanistic understanding of the molecular processes that drive the formation of TDP-43 inclusions may reveal avenues for therapeutic intervention,” the researchers wrote.
Until now, researchers did not have any experimental model that could fully and reliably mimic the behavior of the TDP-43 protein in human disease.
To overcome this limitation, the team developed a new experimental model in which they used a genetically modified version of the TDP-43 protein they called optoTDP43.
The main particularity of this optoTDP42 protein is that it is sensitive to blue light. So when the researchers selectively expose the protein to blue light, they can induce TDP-43 proteinopathy similar to what is seen in human patients.
Using this experimental model, the researchers compared the behavior of a normal TDP-43 protein and three different variants carrying mutations previously identified in ALS patients and known to promote protein aggregation.
Under stimulation with pulses of blue light, optoTDP43 tended to form irreversible aggregates outside the cell nucleus, which is the “command center” of cells and where TDP-43 normally does its work. Interestingly, the optoTDP43 versions that carried the ALS-related mutation exhibited a progressive and faster response, forming more and bigger protein inclusions.
Additional analysis of the underlying binding mechanism revealed that it is mediated by its surrounding environment as well as the particular sequence of TDP-43 protein.
The normal sequence of TDP-43 protein has a small part that can bind to RNA molecules. The researchers found that if this small protein domain is linked to an RNA particle, it will prevent the TDP-43 protein from binding to other TDP-43 proteins and drive the formation of clusters.
Using their experimental model, they saw that RNA-deficient optoTDP43 proteins formed inclusions at a significantly faster rate than RNA-binding competent optoTDP43 versions.
Next, the team tested their optoTDP43 model in human-derived nerve cells. Once again, upon stimulation with blue light, the modified optoTDP43 protein would aggregate. Importantly, these aggregates were found to be toxic to the nerve cells, inducing their degeneration and, ultimately, death.
Since they had previously found that this behavior could be modulated by the RNA-biding ability of the protein, they designed a specific small RNA molecule (oligonucleotide) enhanced for TDP-43 targeting.
“Instead of targeting the gene that causes disease in a subset of patients, we’re targeting the proteins that clump in nearly all of them. That’s never been done before,” Christopher Donnelly, PhD, scientific director of the LiveLikeLou Center for ALS Research at the University of Pittsburgh Brain Institute and senior author of the study, said in a press release.
“We call them ‘bait-oligonucleotides,’ ” Donnelly said. “If you’re fishing, you’re trying to use bait to trap the fish. In our case, we’re leaving the bait there for the extra protein to keep it from clumping together,” said Donnelly, who is also an assistant professor of neurobiology at the University of Pittsburgh.
When they exposed the human nerve cells carrying the optoTDP43 protein to these RNA oligonucleotides, they could not only prevent protein aggregates from forming, but also protect the cells from their toxic effects.
“Collectively, these studies provide insight into the mechanisms that underlie TDP-43 proteinopathy and present a potential avenue for therapeutic intervention,” the researchers wrote.
They are planning to further explore the properties of toxic TDP-43 aggregates and its related downstream mechanisms that contribute to neurodegeneration.


Romano
Sounds promising, also for related diseases such as fosmn. Fingers crossed once more!